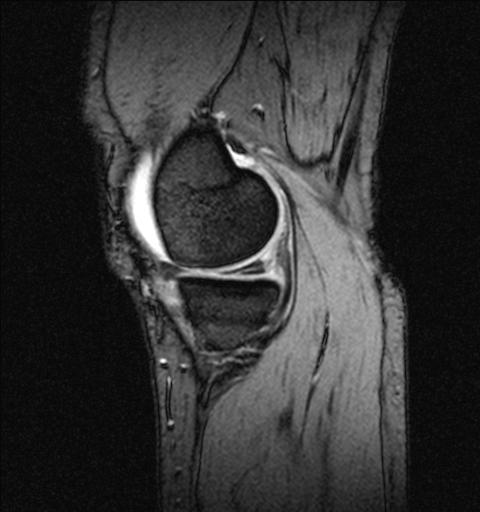
MRI of Knee showing a tear of the Medial Meniscus.The meniscus has a triangular appearance which is changed when the structure is damaged – split horizontally here.
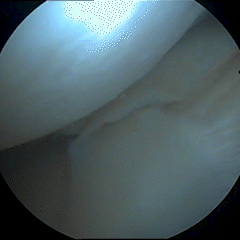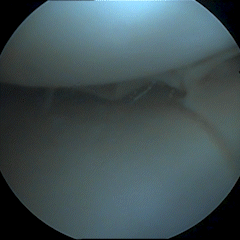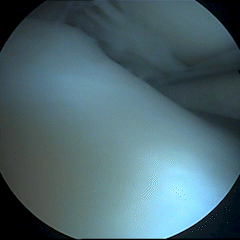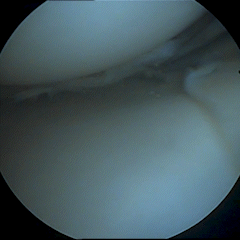
Meniscal tear- Unstable cartilage pieces pull on lining of the joint causing pain and mechanical symptoms such as locking or catching.
Arthroscopy For Cartilage Damage
What is Knee Arthroscopy?
Knee arthroscopy is a common surgical procedure in which the knee joint is viewed using a small high definition camera. This allows the diagnosis and treatment of a range of knee conditions.
What does Knee arthroscopy involve?
Arthroscopy is done through small incisions (keyhole surgery).
During the procedure a small telescope about the size of a pencil is inserted into your knee joint. The high definition camera attached to this arthroscope sends the image to a high resolution television monitor.
Structures of the knee can be seen and tested in great detail.
Using small specialised surgical instruments inserted through other incisions around your knee Mr Jennings can use arthroscopy to feel, repair or remove damaged tissue.
The surgery usually takes between 30 and 60 minutes to complete and is carried out under general anaesthetic as a day case procedure. Prior to your surgery details of your treatment and recovery will be discussed with you by Mr Jennings.
What is a torn cartilage?
There are two meniscal cartilages in the knee. The inner (medial) or outer (lateral) meniscus. These are made of specialised collagen fibres and act to spread the load through the knee, as a sort of shock absorber.
The meniscus can be torn or damaged leading to mechanical irritation of the knee. The cartilage itself has no nerves in it but it is attached to the lining of the knee which is very sensitive. If the damaged cartilage pulls on the sensitive lining it will cause pain. Occasionally big tears may cause mechanical problems, such as giving way and lack of extension (when the knee cannot go straight or is “locked).
Treatment can be either through pain relief and rehabilitation or by surgery to either repair the cartilage or remove the damaged parts causing the irritation. All treatment options will be discussed in full with you. Often the information from an MRI scan can help steer you to the best management plan to suit your symptoms and needs. Repair of the cartilage often requires a slower recovery and protecting the cartilage in a knee brace for several weeks.
What happens after surgery?
After surgery you will have a bandage on your knee that will be changed for a tubigrip (elasticated) dressing after a day. The tubigrip can be removed when any swelling has subsided.
Your incisions will be protected with waterproof dressings that should be left until review in outpatient clinic.
The local anaesthetic injection into the joint at surgery wears off approximately 8 to 12 hours after the surgery. You may notice a gradual increase in pain at this time. Rest, elevation, ice and pain medication are all helpful in relieving pain for the first 1 to 2 days after surgery. On discharge from hospital you may be provided with a prescription for some painkillers which you can use when this occurs. The prescription painkillers will be quite strong and should be used when the knee is very uncomfortable. If the pain is relatively mild then a non-prescription tablet such as paracetamol can be used.
Pain the day after surgery usually occurs with activity and a quiet day at home should be planned. Too high an activity level soon after surgery can prolong recovery time and cause unnecessary setbacks.
Your recovery program will start immediately and will be tailored to your surgery and requirements. You will be instructed on basic self-directed exercises for the immediate post-operative period. In most cases you will walk out of the hospital.
Keep wounds clean, dry, and covered at all times until outpatient review. The waterproof dressing will allow showering but not bathing/immersion.
Mr Jennings will go through details of your surgery before your discharge and will go over this again when you return to the out-patient clinic for review approximately 2 week later.
Rehabilitation
Rehabilitation starts immediately after surgery.
- Tense your thigh muscle (quadriceps for 10 seconds then relax for 10 seconds). Repeat for two minutes every waking hour
- Ankle movement exercises to prevent blood pooling in the calf. Move toe from fully pointed down to up for 2 to 3 minutes every hour
- Straight leg raising exercises to 45 degrees, 3 sets of 10, three times daily
Physiotherapy
You will be given a referral to a physiotherapist for post-operative supervised rehabilitation. This is to help you regain your movement and strength. You should see the physiotherapist within 4-6 days of leaving the hospital. Usually only 3-5 visits are required, with the physiotherapist teaching exercise routines that are appropriate for your age and activity level
When can I Return to work?
This will depend on the nature of your work and activity level. Most patients return to office work 2 weeks after their operation but can work from home after 2 or 3 days. Some more physically demanding jobs may require longer off work.
When can I return to sport?
Most patients are able to return to sporting activity within 3 to 6 weeks in a graduated fashion. Your knee condition and treatment plan will be discussed in detail with respect to your specific case.
Your recovery may be slower if there is more than one knee problem being treated.
When can I drive?
You can get back to driving when you are comfortably walking unaided. You must have sufficient strength to control the foot pedals and be able to perform an emergency stop.
It is a good idea to check the terms of your car insurance to ensure your cover is valid, as some policies state that you must not drive for a specific time period after an operation.
In general terms, this is about 4 to 6 days from arthroscopy. Prolonged journeys are not recommended for at least 14 days from of surgery.
When can I fly?
There is no universal agreement as to when it is safe to travel by plane after knee arthroscopic surgery.
I advise my patients not to fly for at least 2 weeks before and after straightforward arthroscopic surgery.
Short flights do not seem to be a problem. Long intercontinental flights are a potential problem as there is an increased incidence of spontaneous deep venous thrombosis.
The likelihood of developing postoperative leg blood clots depends on many different factors, including your general health, medical history, postoperative mobility and a number of risk factors (obesity, smoking, a history of DVT, etc.).

MRI of Knee showing a tear of the Medial Meniscus.The meniscus has a triangular appearance which is changed when the structure is damaged – split horizontally here.

Meniscal tear- Unstable cartilage pieces pull on lining of the joint causing pain and mechanical symptoms such as locking or catching.






